Cancer screening technology has come a long way, giving doctors powerful tools to detect tumors early when treatment works best. Two leading options—PET-CT and whole body MRI—each bring unique strengths to cancer detection, but choosing between them can feel overwhelming.
This guide is for patients, caregivers, and healthcare professionals who want to understand which screening method might work better for specific situations. We’ll break down how each technology actually works and compare their diagnostic accuracy so you can have informed conversations with your medical team. We’ll also look at the practical side of things—patient comfort, safety considerations, and cost factors that often influence which test your doctor might recommend.
By the end, you’ll have a clearer picture of when PET-CT might be the better choice versus when whole body MRI could be more appropriate for your cancer screening needs.
Understanding PET-CT Technology for Cancer Detection

How PET-CT combines metabolic and anatomical imaging
PET-CT technology combines two powerful imaging techniques into a single comprehensive scan. The PET component tracks glucose metabolism by detecting radioactive fluorodeoxyglucose (FDG), which cancer cells rapidly take up due to their high energy demands. Meanwhile, the CT portion provides detailed anatomical structures and precise location mapping. This fusion creates a complete picture showing both where abnormal metabolic activity occurs and its exact anatomical position.
Key advantages of detecting active cancer cells
Unlike traditional imaging that only shows structural changes, PET-CT identifies metabolically active cancer cells before they form visible tumors. This early detection capability allows doctors to spot cancer recurrence, assess treatment response, and distinguish between scar tissue and active disease. The technology excels at revealing metastases throughout the body in a single scan, making it invaluable for staging and monitoring treatment effectiveness.
Radiation exposure considerations
| Imaging Type | Radiation Dose (mSv) |
| PET-CT | 14-30 |
| Standard CT | 7-20 |
| Chest X-ray | 0.1 |
Patients receive radiation from both the injected radiotracer and CT scan, totaling approximately 14-30 millisieverts. While this exposure is higher than standard CT scans, it remains within acceptable medical limits for diagnostic procedures. Pregnant women should avoid PET-CT scans, and the benefits must outweigh the risks for each patient.
Typical scan duration and patient preparation
The entire PET-CT process takes 2-4 hours, including preparation time. Patients must fast for 6 hours before the scan and receive the radioactive tracer injection 60-90 minutes prior to imaging. The actual scanning takes 30-60 minutes, during which patients lie still on the table. Blood glucose levels need to be checked beforehand, and diabetic patients may require special preparation protocols to ensure optimal image quality.
Exploring Whole Body MRI Capabilities
Superior soft tissue contrast without radiation
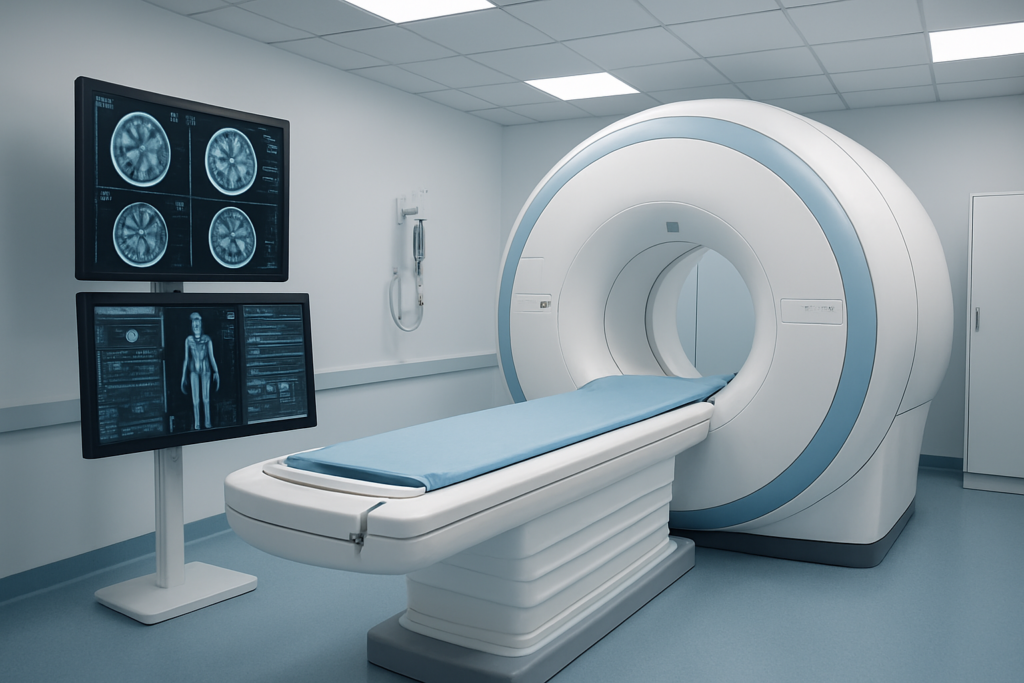
Whole-body MRI excels at distinguishing among different soft-tissue types without exposing patients to ionizing radiation. This magnetic resonance technology uses powerful magnetic fields and radio waves to create detailed images of organs, muscles, and other soft tissues. The absence of radiation makes MRI particularly valuable for screening younger patients or those requiring frequent follow-up scans.
Comprehensive organ visualization in a single session
A single whole-body MRI session can examine multiple organ systems simultaneously, from brain to the pelvis. This comprehensive approach allows radiologists to detect cancer spread across multiple body regions during a single appointment. The technology captures high-resolution images of the liver, pancreas, kidneys, spine, and other critical structures, providing a complete picture of a patient’s health status in approximately 60-90 minutes.
Limitations in detecting small lesions
MRI struggles to detect very small cancerous lesions, particularly those measuring 5-10 millimeters or less. While excellent for soft-tissue contrast, the technology may miss early-stage tumors or microscopic metastases that could be detected by other imaging methods. This limitation becomes especially significant when screening for aggressive cancers that require early intervention for optimal treatment outcomes.
Patient comfort and claustrophobia concerns
The enclosed MRI scanner environment triggers claustrophobia in approximately 15-20% of patients. The lengthy scan duration and loud mechanical noises can cause significant anxiety, sometimes requiring sedation or scan termination. Open MRI systems offer some relief but often compromise image quality. Newer wide-bore scanners and improved patient communication systems help reduce discomfort while maintaining diagnostic capabilities.
Cost implications for healthcare systems
| Cost Factor | Whole Body MRI | Impact |
| Equipment Purchase | $1-3 million | High initial investment |
| Maintenance | $100,000-200,000/year | Ongoing expense |
| Scan Duration | 60-90 minutes | Reduced patient throughput |
| Specialized Staff | MRI technologists required | Higher labor costs |
Healthcare systems face substantial financial challenges in implementing whole-body MRI screening programs. The high equipment costs, specialized staffing requirements, and extended scan times create significant budget pressures. Many facilities struggle to balance the clinical benefits against the economic reality of providing comprehensive MRI screening to large patient populations.
Diagnostic Accuracy Comparison
Sensitivity rates for early-stage cancer detection
PET-CT demonstrates superior sensitivity for metabolically active tumors, detecting early-stage cancers with 85-95% accuracy in most solid tumors. Whole-body MRI excels at identifying structural abnormalities and soft-tissue lesions, achieving 80-90% sensitivity for early detection. Both modalities show varying performance depending on cancer location and size.
Specificity in distinguishing malignant from benign lesions
PET-CT achieves approximately 70-85% specificity, though false positives occur with inflammatory conditions and infections that mimic cancer’s metabolic activity. Whole body MRI demonstrates higher specificity rates of 85-95% through detailed tissue characterization and contrast enhancement patterns, making it particularly effective at distinguishing between malignant and benign masses.
| Imaging Method | Sensitivity Range | Specificity Range | Best Performance |
| PET-CT | 85-95% | 70-85% | Metabolically active tumors |
| Whole Body MRI | 80-90% | 85-95% | Soft tissue masses |
Performance across different cancer types
Lung and colorectal cancers show excellent detection rates with PET-CT due to high glucose metabolism. Brain tumors, liver lesions, and bone metastases respond better to MRI’s superior soft tissue contrast and multiplanar imaging capabilities. Lymphoma screening favors PET-CT, while prostate and gynecological cancers benefit from MRI’s detailed anatomical visualization.
Patient Safety and Comfort Analysis
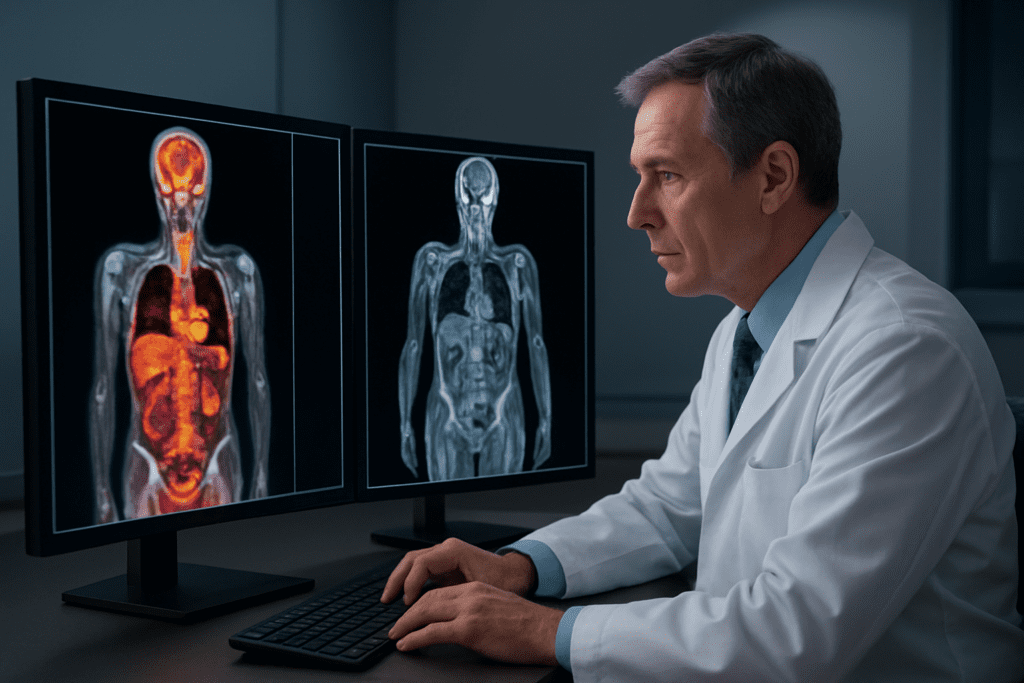
Radiation Risks of PET-CT vs Radiation-Free MRI
PET-CT scans expose patients to significant ionizing radiation, typically 25-30 millisieverts per examination – roughly equivalent to 1,000 chest X-rays. This radiation dose carries a small but measurable cancer risk, particularly concerning for younger patients or those requiring multiple screenings. The radioactive tracer (usually FDG) adds additional exposure beyond the CT component.
Whole body MRI operates without any ionizing radiation, using powerful magnetic fields and radio waves instead. This makes MRI completely safe for repeated screenings without cumulative radiation exposure. Pregnant women and children can undergo MRI examinations without radiation concerns, though specific safety protocols still apply.
Contrast Agent Requirements and Allergic Reactions
| Imaging Type | Contrast Agent | Allergy Risk | Kidney Function Impact |
| PET-CT | Radioactive FDG + CT contrast | Low to moderate | Moderate (CT contrast) |
| Whole Body MRI | Gadolinium-based | Very low | Low to moderate |
PET-CT requires radioactive glucose (FDG) injection plus often iodinated contrast for the CT portion. Iodine-based contrast agents can trigger allergic reactions in sensitive patients and may affect kidney function. MRI uses gadolinium contrast agents, which have significantly lower allergic reaction rates but still require caution in patients with severe kidney disease.
Scan Time Differences and Patient Experience
PET-CT examinations typically take 30-45 minutes total, including preparation time and actual imaging. Patients must fast beforehand and wait about an hour after FDG injection before scanning begins. The procedure involves lying still in a relatively open scanner environment.
Whole body MRI scans require 45-90 minutes of continuous imaging time. Patients experience loud knocking sounds and must remain motionless in a confined tube-like space. Many people find MRI more challenging due to claustrophobia, noise levels, and extended scan duration, though newer open MRI systems help address comfort concerns.
Cost-Effectiveness and Accessibility Factors
Initial Equipment Investment and Maintenance Costs
PET-CT scanners cost between $2-4 million initially, while whole body MRI systems range from $1-3 million. PET-CT requires ongoing expenses for radioisotope production and specialized staff training. MRI systems need regular helium refills and magnet maintenance, but generally have lower operational costs.
Long-term Healthcare Cost Implications
PET-CT’s precision in detecting active cancer can reduce unnecessary procedures and treatments, potentially saving healthcare costs over time. Whole-body MRI may identify more incidental findings requiring follow-up, thereby increasing downstream costs. The cost-effectiveness depends on patient risk factors and the ability to detect cancers at treatable stages.
Clinical Recommendations for Optimal Screening Choice

Patient-specific factors influencing modality selection
Individual patient characteristics play a crucial role in determining the most appropriate screening method. Age, medical history, and existing health conditions directly impact safety and imaging effectiveness. Patients with kidney disease may face restrictions with PET-CT contrast agents, while those with metal implants often cannot undergo MRI scanning. Claustrophobic individuals typically tolerate PET-CT better than the confined MRI environment. Radiation sensitivity, particularly in younger patients and pregnant women, makes whole body MRI the preferred choice for repeated screening protocols.
Cancer type considerations for screening method
Different cancer types respond better to specific imaging modalities based on their metabolic characteristics and anatomical presentation. PET-CT excels at detecting highly metabolic tumors like lung, colorectal, and lymphoma, while whole body MRI provides superior soft tissue contrast for brain, liver, and bone marrow malignancies. Breast and prostate cancers benefit from MRI’s detailed tissue differentiation, whereas head and neck cancers often require PET-CT’s metabolic information for accurate staging and treatment planning.
| Cancer Type | Preferred Method | Key Advantage |
| Lung | PET-CT | High metabolic activity detection |
| Brain | MRI | Superior soft tissue contrast |
| Breast | MRI | Detailed tissue differentiation |
| Lymphoma | PET-CT | Metabolic response assessment |
| Liver | MRI | Enhanced contrast resolution |
Integration strategies for comprehensive cancer surveillance
Modern cancer screening programs increasingly combine both modalities to maximize diagnostic accuracy and minimize individual limitations. Sequential screening protocols use MRI for initial anatomical assessment followed by targeted PET-CT for metabolically suspicious lesions. This approach reduces overall radiation exposure while maintaining diagnostic sensitivity. Hybrid screening schedules alternate between modalities annually, allowing comprehensive surveillance while managing costs. Some specialized centers employ same-day protocols where MRI guides PET-CT targeting, creating a synergistic approach that captures both structural and functional abnormalities for complete cancer detection coverage.

When choosing between PET-CT and whole body MRI for cancer screening, both technologies bring unique strengths to the table. PET-CT excels at detecting active cancer cells and monitoring treatment response, while whole body MRI offers superior soft tissue detail without radiation exposure. Your decision should factor in your specific risk profile, medical history, and what your doctor recommends based on your individual situation.
The best screening approach isn’t always one-size-fits-all. Talk with your healthcare team about which option makes the most sense for you, considering factors like cost, availability, and your comfort level with each procedure. Remember that early detection saves lives, so the most important step is actually getting screened regularly, regardless of which technology you and your doctor choose.


