PET-CT for Cancer Recurrence: How Early Can It Detect Relapse?
Cancer survivors and their families often worry about recurrence after treatment ends. PET-CT scans offer one of the most advanced ways to catch cancer coming back, but understanding when and how early this technology can spot relapse helps patients make informed decisions about their follow-up care.
This guide is for cancer patients, survivors, and caregivers who want to understand PET-CT surveillance and its role in detecting recurrence. We’ll explore the optimal timing for PET-CT surveillance scans after treatment and examine which cancer types benefit most from this imaging approach. You’ll also learn practical strategies to maximize accuracy while reducing the risk of false results that can cause unnecessary anxiety.
Understanding PET-CT Technology for Cancer Detection
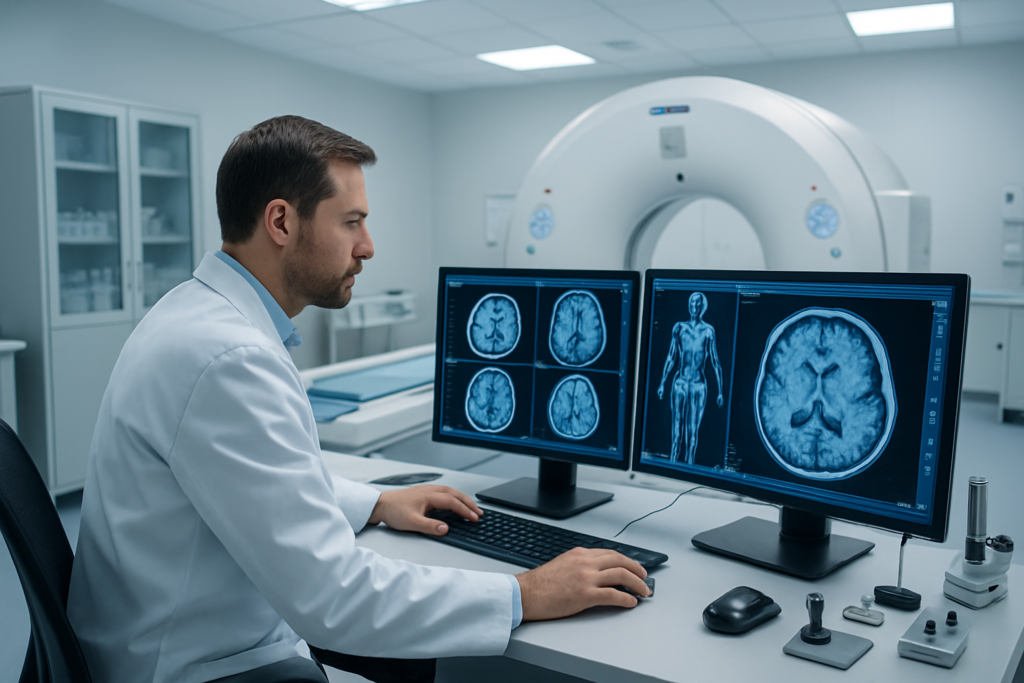
How PET-CT combines metabolic and anatomical imaging
PET-CT combines two powerful imaging technologies into a single comprehensive scan. The PET component tracks glucose metabolism using radioactive tracers, while CT provides detailed structural images of organs and tissues. Cancer cells typically consume glucose at much higher rates than normal cells, making them light up brightly on PET scans. This metabolic activity, combined with precise anatomical mapping, provides a complete picture of the location and biological behavior of cancer cells.
Superior sensitivity compared to conventional imaging methods
PET-CT detects cancer recurrence weeks or months before conventional imaging methods, such as CT or MRI alone. While traditional scans rely on detecting structural changes or tumor size increases, PET-CT identifies metabolic changes that occur much earlier in the disease process. This early detection capability means doctors can spot cancer activity when tumors are still microscopic or before they cause visible anatomical changes, giving patients a significant head start on treatment options.
Timeline for Cancer Recurrence Detection with PET-CT

Earliest Detection Window for Most Cancer Types
PET-CT can identify metabolic changes associated with cancer recurrence as early as 3-6 months after initial treatment, well before structural changes become visible on conventional imaging. This technology detects increased glucose uptake in cancer cells, allowing oncologists to spot recurrent tumors when they’re just 5-10mm in size.
Factors Affecting Detection Sensitivity and Timing
Several key factors influence how quickly PET-CT can detect cancer recurrence. The cancer’s metabolic activity plays the biggest role – highly aggressive tumors with rapid glucose consumption show up faster than slow-growing cancers. Patient factors like blood sugar levels, recent chemotherapy, and inflammation can affect scan accuracy. The location of potential recurrence also matters, as areas with high normal metabolic activity (like the brain or heart) can mask small tumor signals.
| Factor | Impact on Detection |
| Tumor metabolic rate | High activity = earlier detection |
| Blood glucose levels | Elevated levels reduce sensitivity |
| Recent treatment | Can cause false positives |
| Anatomical location | Brain/heart regions more challenging |
Comparison with Other Diagnostic Methods’ Detection Capabilities
PET-CT outperforms traditional CT and MRI scans by 2-4 months in detecting cancer recurrence. While CT scans rely on structural changes and typically catch tumors at 1-2cm, PET-CT identifies metabolic abnormalities at the cellular level. MRI offers excellent soft tissue contrast but lacks the metabolic information that makes PET-CT so effective for early recurrence detection.
Impact of Cancer Stage and Location on Early Detection
The original cancer stage significantly affects PET-CT’s detection capabilities for recurrence. Patients with initially advanced-stage cancers (Stage III-IV) often have better detection rates because their tumors tend to be more metabolically active. Location plays a crucial role – lung, lymph node, and bone recurrences are detected earlier than liver or brain metastases due to varying background metabolic activity in these organs.
Cancer Types Best Suited for PET-CT Surveillance
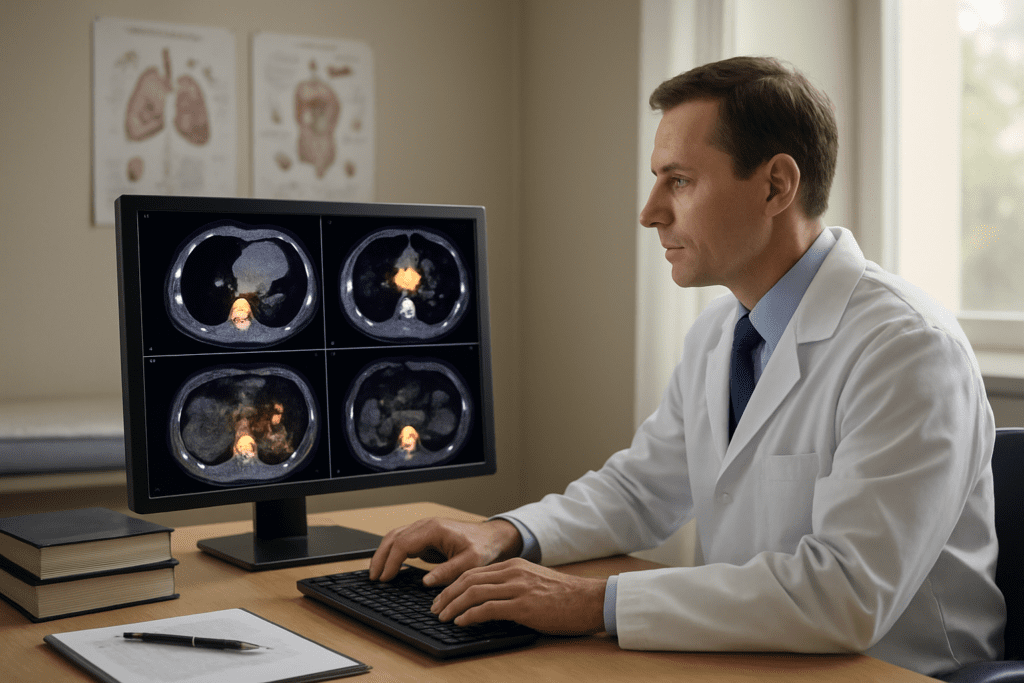
Lymphomas and Blood Cancers with Highest Detection Rates
PET-CT excels at detecting lymphoma recurrence because these cancers show intense glucose uptake, making them light up brightly on scans. Hodgkin lymphoma and aggressive non-Hodgkin lymphomas demonstrate detection rates exceeding 90%, with the ability to spot recurrent disease as small as 5-10mm. The technology proves especially valuable for monitoring treatment response and detecting relapse months before conventional imaging methods.
Solid Tumors with Strong Metabolic Activity
Lung cancer, colorectal cancer, and melanoma respond well to PET-CT surveillance due to their high metabolic activity. These tumors consume glucose rapidly, creating clear contrast against normal tissue. Head and neck cancers also benefit significantly, particularly for detecting recurrence in complex anatomical areas where CT or MRI alone might miss small lesions. Detection sensitivity ranges from 85-95% for most metabolically active solid tumors.
Cancers Where PET-CT Shows Limited Effectiveness
Certain cancers present challenges for PET-CT detection due to low glucose metabolism or anatomical factors. Prostate cancer often shows minimal uptake, making recurrence detection difficult. Brain tumors can be obscured by normal brain glucose activity, while some kidney cancers and well-differentiated thyroid cancers demonstrate insufficient metabolic activity for reliable detection. Mucinous adenocarcinomas also typically show poor PET uptake, limiting surveillance effectiveness.
Optimal Timing for PET-CT Surveillance Scans
Post-treatment monitoring schedules for different cancers
Standard surveillance protocols vary significantly across cancer types. Lymphoma patients typically undergo PET-CT scans at 3-month intervals during the first two years, then transition to 6-month schedules. Lung cancer survivors follow similar patterns, while colorectal cancer monitoring often begins at 6-month intervals from the start. Head and neck cancers require more frequent early surveillance due to higher recurrence rates, with scans every 3-4 months initially.
Risk-based approach to scan frequency
High-risk patients benefit from more aggressive monitoring schedules based on initial staging, treatment response, and molecular markers. Those with complete metabolic response may extend intervals to 6-12 months sooner, while patients showing residual disease or poor prognostic factors maintain tighter 3-month surveillance windows.
Balancing early detection with radiation exposure concerns
Each PET-CT scan delivers approximately 25 millisieverts of radiation exposure. Annual surveillance equates to roughly 100 mSv yearly – significant but manageable when weighed against recurrence detection benefits.
Cost-effectiveness considerations for regular monitoring
PET-CT surveillance costs range from $3,000 to $ 5,000 per scan. While expensive upfront, early recurrence detection enables curative treatments that cost significantly less than managing advanced disease stages.
Maximizing Accuracy and Minimizing False Results
Patient preparation requirements for optimal imaging
Proper fasting for 4-6 hours before PET-CT scanning ensures glucose levels drop, allowing cancer cells to absorb the radioactive tracer more effectively than normal tissues. Patients should avoid strenuous exercise 24 hours prior, as muscle activity can create misleading hotspots that mimic tumor activity.
Understanding false positive and false negative rates
PET-CT demonstrates a false-positive rate of approximately 10-15%, often due to inflammation, infection, or recent surgical sites, which show increased metabolic activity. False negatives occur in 5-10% of cases, particularly with small lesions under 6mm or tumors with low glucose metabolism like certain lung adenocarcinomas.
Combining PET-CT with tumor markers and clinical assessment
| Assessment Method | Sensitivity | Specificity | Best Used For |
| PET-CT alone | 85-90% | 80-85% | Structural changes |
| Tumor markers alone | 60-70% | 70-80% | Biochemical trends |
| Combined approach | 95-98% | 90-95% | Comprehensive evaluation |
Integrating PET-CT results with rising tumor markers like CEA, PSA, or CA-125 provides superior diagnostic accuracy compared to either method alone. Clinical symptoms, physical examination findings, and patient history create a complete picture that reduces diagnostic uncertainty.
When additional confirmatory testing becomes necessary
Biopsy confirmation becomes essential when PET-CT shows equivocal findings, particularly in areas with known inflammatory conditions or previous radiation treatment. Additional imaging modalities like MRI or CT-guided sampling help distinguish between treatment-related changes and true recurrence, especially when clinical suspicion remains high despite negative initial results.
Clinical Benefits of Early Recurrence Detection
Improved Treatment Outcomes with Earlier Intervention
Early detection through PET-CT scanning dramatically changes the cancer treatment landscape. When recurrence is caught in its earliest stages, oncologists can deploy targeted therapies that are significantly more effective than waiting until the disease progresses. Studies consistently show that patients whose recurrences are detected early experience better response rates and longer overall survival times.
Expanded Treatment Options When Cancer is Caught Early
The window of opportunity for treatment options widens considerably with early detection. Surgical resection becomes viable when tumors are small and localized, while radiation therapy can precisely target minimal disease burden. Advanced immunotherapies and precision medicine approaches work best when cancer cell populations are smaller and haven’t developed extensive resistance mechanisms.
Quality of Life Advantages for Patients and Families
Beyond survival statistics, early detection provides profound psychological benefits. Families experience less anxiety when cancer is caught before symptoms appear, and patients maintain better physical function throughout treatment. The ability to address recurrence proactively rather than reactively reduces the emotional toll on everyone involved while preserving patients’ ability to continue normal daily activities during treatment.
PET-CT scans have revolutionized how doctors catch cancer coming back, often spotting trouble months before traditional imaging methods. The technology works best for certain cancer types like lung, colorectal, and lymphomas, where it can detect recurrence as early as 3-6 months after treatment ends. Getting the timing right makes all the difference – too early and you might get misleading results from inflammation, too late and you’ve missed the window for easier treatment.
The real game-changer is how early detection opens up more treatment options and better outcomes for patients. When cancer is caught in its early stages of return, doctors can act quickly with targeted therapies or surgery before it spreads further. If you’re a cancer survivor, talk to your oncologist about whether PET-CT surveillance makes sense for your specific situation and cancer type. The peace of mind that comes from knowing you’re monitoring your health with the most advanced tools available can be just as valuable as the medical benefits themselves.


